Ibogaine offers a powerful experience that attracts those seeking miracles, but it also attracts those seeking to be the beholders of miracles.
Just a Dash of Death
My first encounter with the ibogaine community nearly killed me, but it also saved my life. This exemplifies the juxtaposition inherent in ibogaine community dynamics. Ibogaine offers a powerful experience that attracts those seeking miracles, but it also attracts those seeking to be the beholders of miracles. Many working in the ibogaine world have spent long years suffering through destructive behaviors while also searching for purpose and meaning, and what better path to finally harness for your life’s work than the one that changed your own life. But the line between providing healing to others and holding tyrannical power over others is easily blurred in a community where one might almost conclude that mental instability and unaddressed trauma are required qualifications for the job.
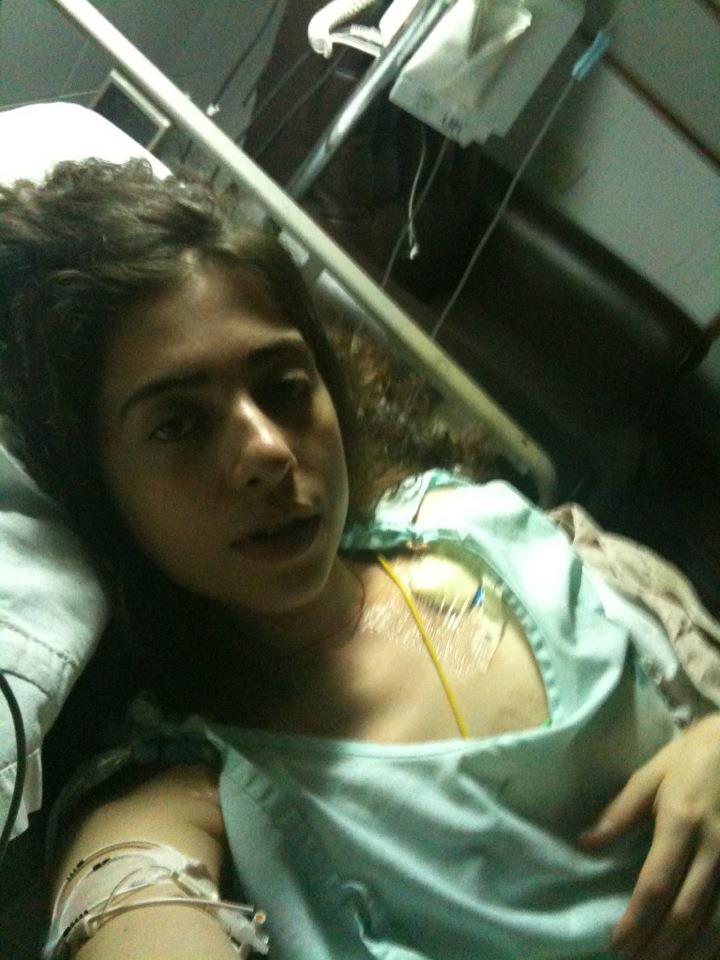
I am one of the many people who became an evangelical ibogaine advocate and aspiring provider. After seven years of opioid dependency, and many other years suffering with depression and anxiety, ibogaine treatment was pretty much the only treatment I hadn’t tried. Although my treatment was a success, in that I left opioids behind for good, I also ended up in an ICU in Guatemala City for ten days on an external pacemaker after experiencing six cardiac arrests. The guys providing my treatment were not following proper safety protocols, and this isn’t a unique occurrence in the world of ibogaine clinics and ceremonies, most of which operate out of the bounds of any governing body. Regardless, the benefits I experienced from the medicine were so profound that I knew I wanted to work with this substance. Discovering that your life of disaster and suffering is suddenly transformed into a kind of priceless training or internship (as I like to refer to my opioid using years) is quite the golden discovery. Working in ibogaine as a former substance-dependent person offers this deep sense of purpose and meaning.
As I was introduced to the community of ibogaine providers, researchers, and doctors in 2012 at my first GITA (Global Ibogaine Therapy Alliance) conference in Vancouver, the reasons behind my hospitalization in Guatemala became obvious. The cardiotoxic effects of ibogaine mean that pretreatment screening, intensive medical monitoring, and diligent adherence to the clinical safety protocols is non-negotiable. The clinic I was treated at in Guatemala made a number of mistakes that became crystal clear as I watched presentations from Dr. Ken Alper, a psychiatrist and researcher at NYU, and others. But research, case reports, and science alone aren’t enough to stop dangerous practices in a community that operates outside of borders, the law, and any kind of supervision process.
Insta-Shaman
Although many make claims that ibogaine is “like 10 years of therapy in one night,” it cannot instantly erase a lifetime of trauma and unhealthy patterns, and it certainly does not “cure” serious mental health issues. Don’t get me wrong; ibogaine is an amazingly powerful medicine, and none of the other treatments I tried for my opioid dependency came anywhere close. The so-called “resetting mechanism” of ibogaine isn’t completely understood scientifically, but there is no denying it once you have experienced it. Waking up in the ICU in Guatemala, I literally felt like I had shed my old self and stepped into a new life altogether. I found my mission in life, was excited and inspired about my new path, and seemingly, like magic, I skipped the crushing fentanyl withdrawal I had coming to me. But, while I left my old destructive relationship with substances behind, the experiences from my childhood still dictated my emotional reactions. The unraveling of life long patterns and behaviors was only beginning for me. Ibogaine is an amazing tool, but it’s merely a door opener.
The following days, weeks, and even months after stepping out of a drug dependency with the help of ibogaine can be a magical time when you experience a connection with life that maybe hasn’t been felt since childhood. It’s so magical that many decide that the right thing to do is to open up an ibogaine clinic immediately, or to go work at one that already exists, without taking time to do internal work or just to learn how to live without chaos. Suddenly, you’re on a God-given mission to help others. You might even imagine that you have a new psychic ability to “save” others. Quite abruptly, you have gone from longing and searching for something that’s missing in your own life to believing you’re the person who is going to deliver people from their own arduous longing for purpose.
The explosive enthusiasm to work in ibogaine isn’t just about finding “your calling”; it’s also born out of an anxiety-driven sense of urgency to find the next external thing that will make your life complete.
The issue latent within this, is that weeks or even months is not sufficient time to process the internalized abusive patterns that have been absorbed from the patriarchal, colonizing, and White Supremacist societies that many of us are raised in. Not only is it not enough time, but it’s probably not going to happen at all without a serious willingness to self-reflect and without the right therapeutic support. The explosive enthusiasm to work in ibogaine isn’t just about finding “your calling”; it’s also born out of an anxiety-driven sense of urgency to find the next external thing that will make your life complete. This is one of the ultimate curses of modern society: We are programmed to believe that material items, other people, drugs, or a certain career is what makes us complete and whole. This desperate seeking, and the clinging onto ideals despite clear warning signs, does not go away with ibogaine. In fact, without the right guidance and support, ibogaine can make it worse. In other words, ibogaine can cause ego-potentiation.
Stepping into the role of “healer” is perfect for anyone with sociopathic or personality disorder traits; you get to have power of others, receive admiration, potentially claim that you’re some kind of prodigy, and actually make money from all of this
The “shaman complex” is a good way to sum this up. What better way to fix years of feeling like the scum of the earth than to suddenly become a person that is praised and looked up to and helps others? Stepping into the role of “healer” is perfect for anyone with sociopathic or personality disorder traits; you get to have power of others, receive admiration, potentially claim that you’re some kind of prodigy, and actually make money from all of this. In this way, an unregulated and unmonitored community can become the perfect grounds for dangerous and unstable people to thrive.
I’m not saying there aren’t talented, stable, and loving people working in the community; there definitely are. But, from what I’ve witnessed, this is not the vast majority and a good portion of the safe practitioners are in fact not men. It’s not cut and dry by gender, and there are unsafe women perpetuating abuses too, but the scariest behaviors I see are perpetrated by the men in the community. Although women suffer from patriarchal societal practices, men are also negatively impacted by them. From a young age, men are taught to hide their true emotions, maintain an appearance of toughness, get recognition at all costs, be a leader, and all of this is what defines who you are. From what I’ve witnessed, it seems that this conditioning can often lead to a terrifying display of power seeking, inability to take responsibility, and self-righteous vigor, all disguised as spirituality and service. Internalized patriarchy can also lead other genders to exhibit these qualities as well, but, because the voices that receive platform in this community have mostly been male, these dangerous behaviors have been most apparent among the men.

Wounded Healers, Wounded Dealings
At the first clinic I trained at, each week, the owner left four to six people (usually predominantly men) under the care of one female nurse for the night of their ibogaine flood, with no doctor or anyone else on site. When I and others in the community raised concerns after witnessing a seizure there, the reaction of the owner was of defensiveness and arrogance. He claimed to have never had a medical emergency and that one would not happen at his clinic, ever. A few years later, a patient died, and many long-time members of the community were not surprised.
Unfortunately, that story is nowhere close to the worst. I have heard multiple accounts of people being left in hotel rooms alone during a flood dose; sometimes, the provider never returns. In one of these stories, a woman woke up in a hospital in Thailand with the provider nowhere to be found, having no idea what happened, and her money gone. There are also many accounts of outright sexual abuse, mostly perpetrated by men upon female clients. A large proportion of clinics are run by men and with a male majority staff. More often than not, women and non-binary folks who come for ibogaine treatment have a history of sexual violence or patriarchal-related trauma. In order to responsibly work with women and other marginalized groups, this would require specialized trauma-based training with a focus on sexual and systemic racial trauma. But this isn’t happening, and there is no body or organization able to enforce responsible practice requirements or to hold people accountable.
Beyond neglectful or unsafe clinical practice and outright physical or sexual abuse, there is also the harder to distinguish psychological and emotional abuse. It can be incredibly hard to identify and take action against this type of abuse, due to the manipulation the perpetrators are often so adept in. The other issue is that it’s difficult to get people to rally in support around victims of this type of abuse, because the perpetrators are so skilled at presenting themselves in different ways to different people. Some are highly regarded in the community but are carefully hiding violent behaviors.
There is also the problem of stigmatization and ostracization between community members. You would think that working in a healing practice would foster only compassion, understanding, and forgiveness; but, unfortunately, the volatile expression of unaddressed trauma carries into the land of ibogaine too. A few years ago, a friend working in Mexico had a relapse which led to some issues in the community. But, instead of a loving intervention, other providers in the nearby community cut off communication and stigmatized him. He has since left the ibogaine world heartbroken, discouraged, and disconnected from the people he had once thought were his family. This story has happened so many times that even in the midst of a dangerous relapse, when life is on the line, people are too petrified of judgment and ostracism to reach out for support in their own community.

Iboga Conservation
Abuse does not just work from person to person, but can be from person to plant, and culture as well. According to the conservation and sustainability organization Blessings of the Forest (BOTF), the rapid popularization of iboga in the West has led to plants being stolen out of protected forests in Gabon leaving traditional Bwiti practitioners no longer able to access their own medicine. There are constantly new iboga sellers popping up online, with no official way to verify that their source is legal or sustainable. There is also the added complication that iboga is not usable as medicine until 5–10 years of growth; so, replenishing plants is no simple task. The best way to guarantee you aren’t using stolen iboga is to use ibogaine converted from voacangine, which is derived from the voacanga tree. This tree grows quickly and plentifully all over West Africa, so it’s a much more sustainable source of medicine. But many practitioners insist on using iboga-derived medicine, often citing that the “spirit of the plant” is missing in voacanga derived ibogaine. I and others have personally witnessed the same transformational experiences with ibogaine derived from voacanga. In my opinion, the “spirit of iboga” is not limited in its ability to show up when it’s called, no matter what plant is used. Applying science-based logic to plant intelligence and spirituality will give us a very narrow and incorrect view of how iboga works. Besides, I imagine the spirit of iboga would greatly appreciate us giving her some time to rest and replenish. Neglecting sustainable sourcing of medicine is a continuation of colonization. At the very least, clinics should be donating back to Gabon, and BOTF, to ensure iboga doesn’t cross into extinction and to safeguard future access to iboga for the traditional peoples who use it as a part of their religion.
Accountability, Safety, and the Future of Ibogaine
Legal regulation, the medical model, and FDA approval are not necessarily the answer for safe psychedelic use. Although aspects of those systems might help in certain situations, there is also reason to believe that this places power in the hands of oppressive governments, a medical system that is often violent and stigmatizing to marginalized populations, and pharmaceutical companies who prioritize profit over people. You might ask: How then can we ensure safe practices and accountability in the ibogaine community?
When GITA was still functional, the publishing of the clinical guidelines in 2015 was a major leap forward. Now, there is a solid, well-researched, and reviewed publication outlining how to facilitate a safe ibogaine treatment. The problem is, there is no way to enforce these protocols and no way to hold practitioners accountable when they aren’t followed. For the most part, clinics operate in places where a client can die and no legal consequences will occur. For example, there was a provider working in Costa Rica who had multiple deaths across multiple Latin American countries and was never held accountable. GITA once offered a grievance process for people needing support around bad clinic experiences, but ways to address the problems with the provider were limited. They could simply choose not to engage in an accountability process.
So, what are the ways to build accountability, responsibility, and better support into the ibogaine world? I am currently a part of the cofounding of a women and genderqueer-led collective for people working in the community called The Root Ibogaine Collective. We are a group formed to promote equity, ethics, safe practices, sustainability, and accountability in the ibogaine community. One idea in development is to offer a training and certification process to clinics that would address clinical safety, but also offer trauma-informed training. One of the requirements for our approval would be that each employee of the clinic be involved in a personal therapeutic process and that a certain percentage of the staff be women. The hope is that, gradually, enough clinics would want to engage in our certification, so that it becomes something that people look for when selecting a clinic. We are also planning to offer weekly meetings and check-ins for providers in order to create a better support system for them.
Psychedelics and Restorative Justice
Deaths, exploitation, and trauma will continue to be perpetuated in our community if we don’t start to set up compassion-driven structures to address harm.
Something else that is much needed, not only in the ibogaine world, but also in the greater psychedelic world in general, is a well-constructed space for accountability and restorative justice processes. So often, the way that harm is dealt with is either using victim blaming and shaming, or the call-out and cancel approach. Both things are rooted in abusive, patriarchal, and colonizing methods of violence. There is a time and place for people to be blacklisted, but more often, there are other routes where healing and education can occur. Deaths, exploitation, and trauma will continue to be perpetuated in our community if we don’t start to set up compassion-driven structures to address harm.

Of course, healing communities attract wounded people, and we all still have work to do on ourselves, and that’s okay. But, if a person is doing harm, and continually refuses to be responsible for it, then a community-led intervention is needed. The hyper-focus of many on getting FDA approval for ibogaine is dangerous, because that will not address the systemic and interpersonal abuses that continue to happen. Before we can spread ibogaine to a larger audience, we must address the dangerous issues we have now.
We can’t discuss systemic violence without discussing interpersonal violence, because what happens in our close relationships creates the materials that build the larger system.
The abuses in the ibogaine community are not just limited to the provider-to-client relationship, but also occur between those who work in the community. One of my main inspirations to write and work on these issues comes from something I recently experienced personally. A person who I collaborated with and was quite close to in the community for many years became very emotionally violent towards me last year. As I watch him receive accolades and respect for his work, he still won’t accept responsibility for this behavior, which is very concerning and painful to witness. We can’t discuss systemic violence without discussing interpersonal violence, because what happens in our close relationships creates the materials that build the larger system. This experience has made it clear to me that new systems need to be in place in the community to support victims of abuse. I would like to call on anyone experiencing harm in the community to speak up about their experiences and ask for support. It’s takes a collaborative community approach and a willingness to be vulnerable to create healing structures that address harm.
Art by Karina Alvarez.